Diabetic Neuropathy
🧾 Introduction
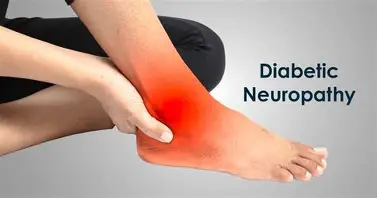
Diabetic neuropathy is a group of nerve disorders caused by prolonged high blood sugar levels in individuals with Diabetes Mellitus. It is one of the most common and serious long-term complications of diabetes, affecting up to 50% of diabetic patients over time.
This condition primarily damages peripheral nerves, especially those in the feet and legs, but it can also involve autonomic and focal nerve systems. If left unmanaged, diabetic neuropathy can lead to severe complications such as foot ulcers, infections, and even amputation.
🧬 What is Diabetic Neuropathy?
Diabetic neuropathy refers to nerve damage resulting from chronic hyperglycemia (high blood glucose levels). Elevated glucose levels impair nerve function directly and damage the small blood vessels (microvasculature) that supply oxygen and nutrients to nerves.
Over time, this leads to:
- Loss of nerve signaling
- Reduced sensation
- Pain or abnormal sensations
⚙️ Pathophysiology (How It Develops)
The development of diabetic neuropathy is multifactorial and involves:
- Metabolic factors: Excess glucose leads to accumulation of sorbitol and oxidative stress
- Vascular factors: Reduced blood flow causes nerve ischemia
- Inflammation: Chronic low-grade inflammation damages nerve fibers
👉 These mechanisms collectively result in progressive nerve degeneration.
⚠️ Types of Diabetic Neuropathy
1. Peripheral Neuropathy
The most common form, affecting:
- Feet and legs (first)
- Hands and arms (later)
Features:
- Numbness
- Tingling (“pins and needles”)
- Burning pain
2. Autonomic Neuropathy
Affects involuntary body functions such as:
- Digestion
- Heart rate
- Blood pressure
- Bladder function
Symptoms:
- Gastroparesis (delayed stomach emptying)
- Dizziness on standing
- Urinary problems
3. Proximal Neuropathy (Diabetic Amyotrophy)
Affects thighs, hips, and buttocks.
Features:
- Sudden severe pain
- Muscle weakness
- Difficulty standing
4. Focal Neuropathy
Involves damage to specific nerves, often sudden in onset.
Examples:
- Cranial nerve palsy
- Carpal tunnel syndrome
🔍 Causes
The primary cause is chronic hyperglycemia, but several contributing factors exist:
- Long-standing diabetes
- Poor glycemic control
- Obesity
- Smoking
- Alcohol use
- Genetic susceptibility
⚠️ Symptoms
Early Symptoms:
- Tingling or burning sensation
- Mild numbness
- Increased sensitivity to touch
Progressive Symptoms:
- Sharp, stabbing pain
- Loss of sensation
- Muscle weakness
Advanced Symptoms:
- Loss of balance
- Foot ulcers
- Infections
🧪 Diagnosis
Diagnosis is primarily clinical, supported by specific tests:
Clinical Examination:
- Sensory testing (touch, vibration, temperature)
- Reflex assessment
Diagnostic Tests:
- Nerve conduction studies
- Electromyography (EMG)
- Monofilament testing
- Blood glucose and HbA1c levels
⚠️ Risk Factors
Modifiable:
- Poor blood sugar control
- Sedentary lifestyle
- Smoking
- Obesity
Non-Modifiable:
- Duration of diabetes
- Age
- Genetic predisposition
⚡ Complications
Diabetic neuropathy can lead to serious complications:
- Foot ulcers
- Infections
- Amputation
- Digestive disorders
- Cardiovascular instability
👉 One of the most severe outcomes is Diabetic Foot, which can result in limb loss.
🥗 Management & Treatment
1. Glycemic Control
Strict control of blood glucose is the cornerstone of treatment.
2. Medications
Used primarily for symptom relief:
- Pain relievers
- Antidepressants (e.g., duloxetine)
- Anticonvulsants (e.g., pregabalin)
3. Lifestyle Modifications
- Healthy diet
- Regular exercise
- Smoking cessation
- Weight management
4. Foot Care (Critical)
- Daily inspection of feet
- Proper hygiene
- Use of protective footwear
- Regular podiatric check-ups
🛡️ Prevention
Preventive strategies focus on controlling risk factors:
- Maintain optimal blood sugar levels
- Regular medical check-ups
- Early detection of symptoms
- Healthy lifestyle practices
👉 Prevention is significantly more effective than treatment.
📊 Quick Summary
| Factor | Key Insight |
|---|---|
| Main Cause | Chronic high blood sugar |
| Most Common Type | Peripheral neuropathy |
| Key Symptoms | Pain, numbness, tingling |
| Major Risk | Poor diabetes control |
| Serious Outcome | Ulcers, amputation |
| Prevention | Glycemic control + lifestyle |
🧠 Clinical Significance
Diabetic neuropathy is not only a quality-of-life issue but also a major contributor to morbidity in diabetic patients. It increases the risk of hospitalization, disability, and healthcare costs.
Early intervention can significantly reduce disease progression and complications.
🧠 Conclusion
Diabetic neuropathy is a progressive and potentially debilitating complication of Diabetes Mellitus, but it is largely preventable and manageable. Through early diagnosis, strict glycemic control, and appropriate lifestyle modifications, individuals can significantly reduce their risk and maintain a good quality of life.
________________________________________________________________________________________________________________________________